Back when I was in college (10+ years ago), a guy I knew had a girlfriend who he didn’t seem to like. One day, I asked why they were still together.
“She has HPV,” he said matter-of-factly.
Excuse me?
“Which means I have it,” he said. “And I don’t want to pass it to anyone else.”
In the moment, twenty-one-year-old me thought okay that kind of makes sense, but no, no it doesn’t. HPV may be a sexually-transmitted infection, but it’s not a Scarlett letter — and it’s not a death sentence!
In fact, women under 30 years old aren’t even tested for HPV anymore. Yes, you read that right! So if you had an HPV diagnosis in your twenties, it was all for naught, my friend.
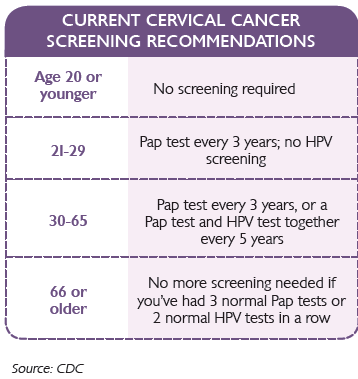
The new guidelines are as follows:
The reason HPV is no longer tested in twenty-somethings is because it’s common, it’s symptomless, it usually goes away on its own, and it requires no treatment.
I can only imagine how many people stayed together or broke up because of an HPV diagnosis… it’s kind of sad, actually.
The fact is: there are many HPV strains and most are harmless. Only 14 are considered high-risk or cancer-causing and just two of those (types 16 and 18) cause 70% of invasive cervical cancers.
Whenever I hear of someone getting a cervical cancer diagnosis, it seems sudden, progressive, and, far too often, deadly.
But here’s what we know: 99.7% of all cervical cancer cases start with a high-risk HPV infection, which means if you get the HPV vaccine and follow the CDC’s screening recommendations, you should be able to prevent it.
In fact, a recent study shows that no cervical cancer cases developed in women who got the full HPV vaccine between ages 12 and 13.
The vaccine may be a reason why we’re seeing lower cervical cancer rates in women ages 20-24 (65% less over the course of seven years). However, rates are starting to rise among women in their 30s and 40s who may or may not have gotten the HPV vaccine — or got the vaccine and therefore skipped the screenings.
Thankfully, 44% of people with cervical cancer are diagnosed at an early stage, giving them a five-year survival rate of 91%. But that means 66% are diagnosed at a later stage… and once cervical cancer has spread to a distant part of the body, it lowers the five-year survival rate to 19%.
This is why, regardless of the fact that I have been with the same partner for eight years and got the vaccine and regular screenings in my twenties (before the recommendations changed), I still follow the CDC screening recommendations.
I’m not worried about HPV — and you shouldn’t be either — but I’d rather be safe than sorry. Plus, checking your cervix on a regular basis is a good practice of self-care.
Ana G. Cepin, MD, is an Associate Professor of Obstetrics & Gynecology at Columbia University Irving Medical Center/NY-Presbyterian Hospital.
Long before she became an ObGyn, Dr. Cepin was super interested in gynecology and reproductive health. In her younger years, she would educate her friends about their menstrual cycles. Now, she spends her day-to-day focused on preventive care, family planning, and general gynecology, with a commitment to advancing health equity.
In our discussion, we tackle HPV, cervical cancer, and why it’s so important to follow screening guidelines.
Q: Why is the HPV vaccine so important?
The data is very compelling that the HPV vaccination decreases the risk of cervical cancer by huge levels [and a new 2024 study found zero cases of cervical cancer among women who were vaccinated before age 14].* It’s very effective and the earlier you get it the better, especially before becoming sexually active and becoming exposed to HPV. The rates of cervical dysplasia which are just changes of the cervix and cervical cancer decrease significantly after vaccination.
Q: Do you have to get all three doses for it to be effective?
There is some protection with just one injection, but really the whole series is needed. Routine vaccination is typically at 11-12 years, but you can be vaccinated until the age of 45. If you have your first injection before the age of 15, only two doses are needed. The good thing is that if you fall off of the schedule a little bit, you can always return and not have to restart the doses; there is some leeway.
Q: A new FDA-approved blood test can now detect HPV, which may eliminate the need for the pap smear.
It looks like this is from menstrual blood. I would say that this is one example of ways to test for HPV without the need for a pap smear and holds promise for the future.
Q: HPV is very common and many people will have it in their lifetime – approximately 13 million Americans will be infected every year. What’s something people should know about HPV that they might not already?
I have this conversation with patients all the time. HPV is super common. Most people will be exposed to it and at some point most people will clear the infection. It usually goes away. With any sexually transmitted infection, there can be stigma associated with it. The other thing that makes HPV challenging, similar to herpes, is that we don't have an effective treatment to eliminate it so that can leave people in a place of limbo where they know that they have this infection, but that there's nothing they can do about it. That's part of what makes it a challenging infection.
Q: How would someone know they have HPV if they don’t get screened?
There are no symptoms. Only if you have cervical cancer will there be symptoms [and those symptoms are here]. This is why the pap smear and HPV testing is so important.
There are also different strains of HPV. There are certain strains that correlate to genital warts that can happen anywhere along the genital area. There are other strains that are associated with cervical cancer and these don’t have any symptoms early on that’s why it’s so important to screen for them.
Q: Even if someone has the same partner for years and years, it’s still important for them to continue with regular pap smears, right?
Yes. You may have an infection that was not necessarily picked up before. We’re not even testing for HPV before the age of 30.** You may not know that you have it, depending on your age, and also the test is not an “all or none” phenomenon. There's a threshold and so your immune system may have been suppressing your infection, which is really great, but if something were to change where your immune system is no longer suppressing it any any longer then there can be a situation where it’s now detected at a higher level.
The HPV infection ICD-10-CM code refers to cervical high-risk HPV, for instance, which means it’s a clinically important infection. [If it’s not high-risk, it wouldn’t be reported in your medical records]. Also, you may trust your partner but that doesn't always mean that you should. If there is exposure elsewhere, that may be passed on to you.
Q: My understanding is there’s no cure for HPV. Is that right?
This is frustrating for patients. There is no medication that we give to treat the infection. That’s very common with viruses. The good news is that our bodies are very effective in fighting off the infection, so the vast majority of cases will resolve on their own. It's just a matter of waiting. However, in a small percentage of women, the infection will not resolve and those are the ones we care about. Those are the ones that can eventually lead to cancer.
Q: If HPV goes away, can it come back?
It’s not that it goes away and comes back. In theory, if you fight off an infection then it goes away, but that’s not always the case. Some women, for example, have been sexually active for years and years and negative for HPV, but then all of a sudden they’re not sexually active, but positive for HPV. The thinking is that the infection was dormant and now it’s active, but the vast majority clear on their own and you end up gaining immunity to it.
If you’re exposed to a strain of HPV, then you’re not going to be at risk for a repeat infection of that strain, but there are dozens of strains so just because you had one and cleared it, it doesn’t mean you’re protected from the others.
Q: Are patients told which strains they have? Does that show up on medical records?
There are dozens and dozens of strains so the ones we’re testing for are the ones associated with cervical cancer. These are what we call high-risk HPV strains. Depending on your laboratory, you likely won’t know which strain you have, you’ll just know that you have it, with the exception of strain 16 and 18, as we know these are the most dangerous, so depending on the lab this may be listed as part of the report.
Q: If you have high-risk strains, what happens next?
Depending on the strain and the pap results you may be advised to repeat the testing in one year or to have a procedure called a colposcopy where we take a closer look at the cervix.
Q: Does cervical cancer take a long time to develop?
There are exceptions to everything, but typically cervical cancer takes decades to develop, so a colposcopy would look to see if cells are precancerous and if you remove those cells early on, it usually prevents cervical cancer from developing. Essentially, everyone should get vaccinated. It’s the best way to prevent an infection.
Cervical cancer is a very preventable cancer, but the one way we can prevent it from developing is to screen for it.
Q: What’s one healthy habit you can’t live without?
I find nature to be very restorative so any chance I get to do things in nature, I tried to do, like hiking.
*Children can get the HPV vaccine as young as nine years old and those over 15 need to get three doses for effectiveness.
**Pap smears are no longer recommended for women under the age of 21 or those who’ve had a hysterectomy for non-cancer disease.
Mind
A new study shows that the brain actually changes during menstruation… I mean, are we surprised? The female body (and brain) is wild.
Body
One-third of pregnant women show signs and symptoms of preeclampsia, according to a new study, but only 14.2% are diagnosed with it. This calls into question are current screenings and diagnostics criteria, which may not sufficiently address the issue.
Beyond
Midi Health, the fastest-growing virtual clinic treating women in perimenopause and menopause, just raised $60 million.
Maven Clinic is now offering “Trying-To-Conceive (TTC) health coaching,” which aims to help those wanting to get pregnant without IVF and will include ovulation tracking kits, regular check-ins, nutritional support, etc.
Funny Story
So, I don’t actually recommend every Emily Henry book, but I am enjoying her latest novel and if you haven’t read her books yet, I suggest starting with Book Lovers or Beach Read.
Maple-flavored walnut milk
While I love oat and almond milk, I think walnut milk is highly underrated (and provides much more nutritional value than oats). This is my current favorite flavor from Elmhurst, but you can’t really go wrong with any of them.
The Circle
My husband and I don’t even like social media that much, but we’re loving this Netflix show… so we went back to season one and it was even better in the beginning than it is now. Highly recommend for those wanting an easy watch.
Did you enjoy this issue? Consider subscribing or sharing with a friend.